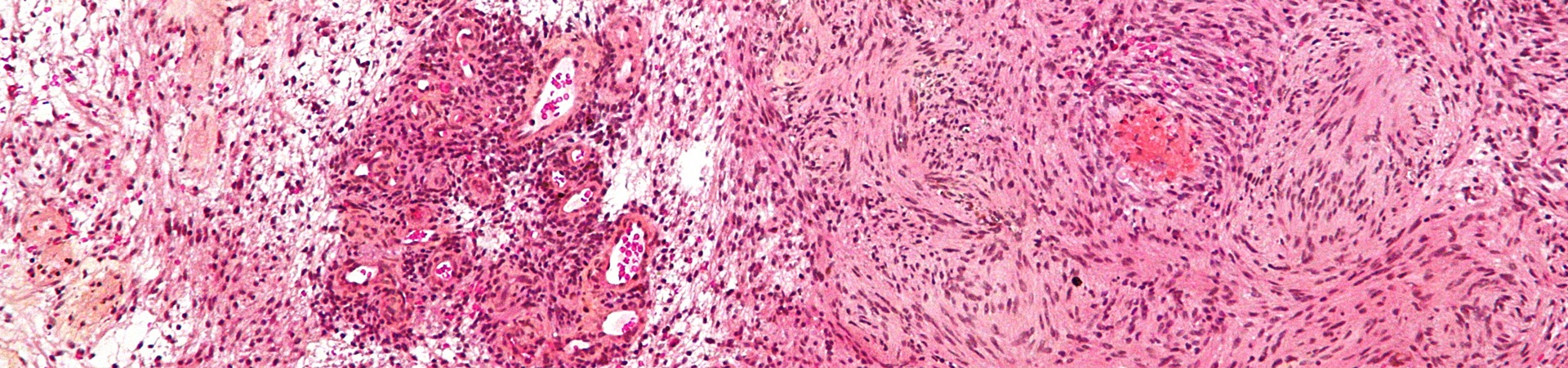
Scwhannomatoses : NF2, SMARCB1, LZTR1 and the others are genetic syndromes predisposing individuals to develop multiple schwannomas, as well as meningiomas and ependymomas, primarily in the context of NF2-related schwannomatosis (1). They are rare diseases, with prevalence varying significantly depending on the causative genetic mutation. The most recent epidemiological data report a prevalence of 1 in 61,332 individuals for NF2-related schwannomatosis, 1 in 527,000 for LZTR1-related schwannomatosis, and 1 in 1.1 million for SMARCB1-related schwannomatosis (2).
Unlike patients with Neurofibromatosis type 1 (NF1), patients with schwannomatoses often experience a diagnostic delay of several years after the onset of initial symptoms. This delay is explained by the rarity of familial forms, where at least one parent is affected, which account for only 23% of NF2-related schwannomatosis cases and 15% of non-NF2-related schwannomatoses. Sporadic forms, in which neither parent is affected, are much more common. Additionally, mosaic forms (50% of sporadic cases), where the phenotype is less severe and more variable, contribute to diagnostic challenges (3). Even within the two clinical forms (familial and sporadic), there exists a subgroup of patients with segmental schwannomatosis, where only a single limb is affected.
Schwannomatoses are linked to mutually exclusive germline mutations in three tumor suppressor genes: NF2, SMARCB1 (4), and LZTR1 (5), all located on chromosome 22. NF2-related schwannomatosis is, as the name suggests, exclusively linked to the NF2 gene. Among non-NF2-related schwannomatoses, SMARCB1 mutations are found in 40–45% of familial cases and 8–10% of sporadic cases, while LZTR1 mutations are present in 30–35% of familial cases and 25–30% of sporadic cases. A significant proportion of familial and sporadic schwannomatoses unrelated to NF2 currently lack an identified genetic cause (6).
In NF2-related schwannomatosis, biallelic loss of the NF2 gene is both necessary and sufficient to initiate tumor formation. In non-NF2-related schwannomatoses, the formation of each schwannoma follows a more complex three-step tumorigenesis mechanism: an initial germline mutation in a tumor suppressor gene (SMARCB1 or LZTR1), followed by somatic inactivation of the second allele on chromosome 22 through loss of heterozygosity (LOH), and finally, a somatic mutation in the NF2 gene, leading to biallelic inactivation of both NF2 and the other schwannomatosis-associated gene.
Patients with schwannomatoses are typically diagnosed between the ages of 18 and 24 for NF2-related schwannomatosis and later, between 20 and 40 years, for non-NF2-related schwannomatoses. NF2-related schwannomatosis most commonly presents with sensorineural hearing loss or, in childhood cases (<16 years), with vision loss (7). Patients exhibit bilateral vestibular schwannomas, intracranial meningiomas in 50% of cases, intramedullary ependymomas, spinal tumors (meningiomas and schwannomas), and peripheral schwannomas. In addition to tumors, patients may develop axonal neuropathies resembling pseudo-Charcot-Marie-Tooth disease, causing significant motor deficits (8).
In non-NF2-related schwannomatoses, the primary symptoms at diagnosis include pain (46%), palpation of a mass (27%), or both (11%). Sensory-motor deficits are rarely present at the initial assessment. Patients predominantly present with peripheral nerve schwannomas (89%) and spinal schwannomas (74%). Cranial nerve schwannomas are rare (8%); unilateral vestibular schwannomas are found in 15% of LZTR1-related schwannomatosis cases, while trigeminal schwannomas occur in other cases. Unilateral vestibular schwannomas, though uncommon, can be observed in patients with schwannomatoses. Intracranial meningiomas are also rare (5%), appearing exclusively in SMARCB1-related schwannomatoses, predominantly along the falx (9).
Initial imaging evaluation includes a brain MRI with fine slices centered on the internal auditory canals, a whole-spine MRI, and additional MRIs targeting painful regions based on each patient's presentation. If feasible, whole-body imaging (MRI or PET-MRI) (10) is recommended at the initial evaluation. Subsequent MRI follow-ups are conducted annually or biennially, depending on tumor burden. The radiological appearance of schwannomas in schwannomatosis patients is similar to that of sporadic schwannomas, except for multinodular forms, resulting from the fusion of multiple contiguous schwannomas along a single peripheral nerve, which are notably present in vestibular schwannomas (11). High-resolution MRI neurography can also reveal multiple intrafascicular microlesions along peripheral nerves (12). These microlesions are present throughout the limbs in segmental schwannomatosis, where macroscopic schwannomas and pain are confined to a single limb. There is no definitive link between these microlesions and patient-reported pain. Furthermore, electrophysiological studies are typically normal in schwannomatosis patients (13).
Schwannomatosis patients receive care in specialized "rare disease" centers that integrate clinical management with genetic counseling. Clinically, management in NF2-related schwannomatosis focuses on preserving neurosensory functions, whereas in non-NF2-related schwannomatoses, the priority is pain management. Unlike NF1, malignant transformation is exceedingly rare in schwannomatoses, usually associated with prior radiation therapy (14), and therefore, cancer prevention is not a primary concern.
In NF2-related schwannomatosis, preserving hearing is a key therapeutic goal, achieved through a combination of surgery (vestibular schwannoma resection, internal auditory canal decompression), radiosurgery, and chemotherapy (Avastin, Everolimus, Brigatinib) (15–17). When hearing loss occurs, restoration options include cochlear or brainstem implants. Other neurological functions, such as motor control, sensation, vision, and speech, may be impaired, necessitating tumor-specific surgical intervention (intracranial or spinal meningioma, intramedullary ependymoma, or spinal schwannoma).
In non-NF2-related schwannomatoses, pain management, affecting 68% of patients, is the primary focus. Pain presents as episodic attacks, sometimes with a continuous baseline pain, and may or may not be associated with an underlying schwannoma (9). Initial treatment is medical, though refractory pain is common; 27% of patients report using more than six pain medications (9). Surgery is reserved for rapidly growing tumors or those explicitly causing symptoms. Peripheral schwannoma surgery in schwannomatosis patients yields slightly lower pain relief rates than in sporadic cases (85%). Additionally, post-operative deficits occur more frequently (33%), particularly in patients with multi-segmental disease or undergoing resection of multiple tumors in a single procedure (18). To date, the effects of radiotherapy and chemotherapy in treating non-NF2-related schwannomatoses remain limited.
The natural history of the disease includes the emergence of new meningiomas and schwannomas over time (18). It remains unclear whether this is due to incomplete initial assessment—since whole-body MRI is not routinely performed—or actual tumor progression. Malignant transformation of peripheral schwannomas has been reported in schwannomatoses (18), primarily in SMARCB1-related forms and very rarely in NF2-related schwannomatosis, though its true prevalence remains uncertain due to diagnostic revisions in reference pathology series (9).
Michel Kalamarides
Referral centre for neurofibromatosis type 2 and schwannomatosis
AP-HP - Pitié-Salpêtrière Hospital - 75013 - Paris - France
Matthieu Peyre
Sorbonne University – Neurosurgery department
AP-HP – Pitié-Salpêtrière Hospital – 75013 – Paris – France
- MacCollin M, Woodfin W, Kronn D, Short MP. Schwannomatosis: a clinical and pathologic study. Neurology. 1996 Apr;46(4):1072–9.
- Evans DG, Bowers NL, Tobi S, Hartley C, Wallace AJ, King AT, et al. Schwannomatosis: a genetic and epidemiological study. J Neurol Neurosurg Psychiatry. 2018 Jun 16;
- Halliday D, Emmanouil B, Pretorius P, MacKeith S, Painter S, Tomkins H, et al. Genetic Severity Score predicts clinical phenotype in NF2. J Med Genet. 2017 Oct;54(10):657–64.
- Hulsebos TJM, Plomp AS, Wolterman RA, Robanus-Maandag EC, Baas F, Wesseling P. Germline mutation of INI1/SMARCB1 in familial schwannomatosis. Am J Hum Genet. 2007 Apr;80(4):805–10.
- Piotrowski A, Xie J, Liu YF, Poplawski AB, Gomes AR, Madanecki P, et al. Germline loss-of-function mutations in LZTR1 predispose to an inherited disorder of multiple schwannomas. Nat Genet. 2014 Feb;46(2):182–7.
- Hutter S, Piro RM, Reuss DE, Hovestadt V, Sahm F, Farschtschi S, et al. Whole exome sequencing reveals that the majority of schwannomatosis cases remain unexplained after excluding SMARCB1 and LZTR1 germline variants. Acta Neuropathol (Berl). 2014 Sep;128(3):449–52.
- Halliday D, Emmanouil B, Vassallo G, Lascelles K, Nicholson J, Chandratre S, et al. Trends in phenotype in the English paediatric neurofibromatosis type 2 cohort stratified by genetic severity. Clin Genet. 2019 Aug;96(2):151–62.
- Peyre M, Tran S, Parfait B, Bernat I, Bielle F, Kalamarides M. Surgical Management of Peripheral Nerve Pathology in Patients With Neurofibromatosis Type 2. Neurosurgery. 2023 Feb 1;92(2):317–28.
- Merker VL, Esparza S, Smith MJ, Stemmer-Rachamimov A, Plotkin SR. Clinical features of schwannomatosis: a retrospective analysis of 87 patients. The Oncologist. 2012;17(10):1317–22.
- Ahlawat S, Fayad LM, Khan MS, Bredella MA, Harris GJ, Evans DG, et al. Current whole-body MRI applications in the neurofibromatoses: NF1, NF2, and schwannomatosis. Neurology. 2016 Aug 16;87(7 Suppl 1):S31-39.
- Stivaros SM, Stemmer-Rachamimov AO, Alston R, Plotkin SR, Nadol JB, Quesnel A, et al. Multiple synchronous sites of origin of vestibular schwannomas in neurofibromatosis Type 2. J Med Genet. 2015 Aug;52(8):557–62.
- Farschtschi S, Mautner VF, Pham M, Nguyen R, Kehrer-Sawatzki H, Hutter S, et al. Multifocal nerve lesions and LZTR1 germline mutations in segmental schwannomatosis. Ann Neurol. 2016 Oct;80(4):625–8.
- Schulz A, Grafe P, Hagel C, Bäumer P, Morrison H, Mautner VF, et al. Neuropathies in the setting of Neurofibromatosis tumor syndromes: Complexities and opportunities. Exp Neurol. 2018;299(Pt B):334–44.
- Evans DG, Halliday D, Obholzer R, Afridi S, Forde C, Rutherford SA, et al. Radiation treatment of benign tumors in NF2-related-schwannomatosis: A national study of 266 irradiated patients showing a significant increase in malignancy/malignant progression. Neuro-Oncol Adv. 2023;5(1):vdad025.
- Plotkin SR, Stemmer-Rachamimov AO, Barker FG, Halpin C, Padera TP, Tyrrell A, et al. Hearing improvement after bevacizumab in patients with neurofibromatosis type 2. N Engl J Med. 2009 Jul 23;361(4):358–67.
- Plotkin SR, Yohay KH, Nghiemphu PL, Dinh CT, Babovic-Vuksanovic D, Merker VL, et al. Brigatinib in NF2-Related Schwannomatosis with Progressive Tumors. N Engl J Med. 2024 Jun 27;390(24):2284–94.
- Goutagny S, Giovannini M, Kalamarides M. A 4-year phase II study of everolimus in NF2 patients with growing vestibular schwannomas. J Neurooncol. 2017 Jun;133(2):443–5.
- Gonzalvo A, Fowler A, Cook RJ, Little NS, Wheeler H, McDonald KL, et al. Schwannomatosis, sporadic schwannomatosis, and familial schwannomatosis: a surgical series with long-term follow-up. Clinical article. J Neurosurg. 2011 Mar;114(3):756–62.